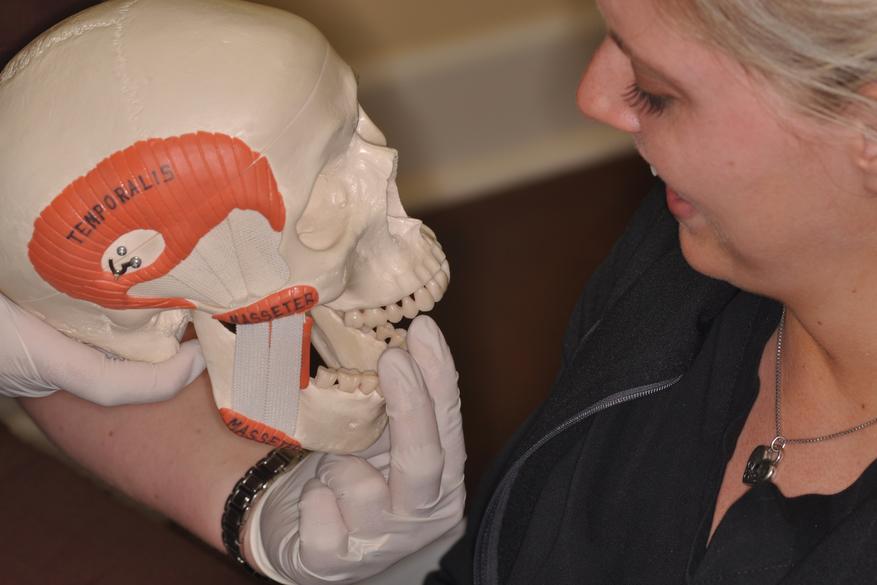
TMJ
Ever since learning about TMJ in dental school Dr. Shannon developed a deep passion for helping people afflicted with this series of disorders. One of the main reasons Dr. Shannon chose to complete a prosthodontic residency after dental school was because the prosthodontic specialty was the only recognized dental specialty that required extensive training in TMJ. There was no true recognized dental specialty in “TMJ”. Most dentist get little education in TMJ while in dental school and must educate themselves afterwards through continuing education courses if they are interested in treating the disorder. Prosthodontics was the only true dental specialty that includes treating TMJ as part of the specialty. Recently since 2020 TMJ has finally become a specialty of its own and is now one of the ADA recognized dental specialities.
Dr. Shannon has been treating TMJ for the past 21 years in residency and private practice. In addition to private practice he has been the director of the LSU School of Dentistry TMJ/TMD Orofacial Pain Clinic for the past 12 years. Dr. Shannon also teaches at the dental school and has been director for the Temporomandibular Disorders course that the dental students take in their third year of school for the past 12 years. He is also director of the senior dental student TMD clinic rotation for the past 12 years.
Dr. Shannon is a member of several national dental societies that devote themselves to the diagnosis and treatment of TMJ. He attends annual meetings and keeps up with the latest research and advancements in the field of TMJ in order to provide the most up to date treatment based on the latest research for his patients. Unfortunately there is no regulation on the treatment of TMJ. Almost anyone can claim to treat TMJ in any way they seem fit. It is essential for patients to be very cautious when seeking treatment as there are many outlandish, irreversible, expensive treatments to stay away from. Beginning treatment should always be very conservative.
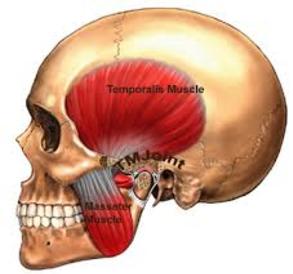
TMJ is actually three letters that stand for the temporomandibular joint. It is our jaw joint. So, we all have TMJ. We have two TMJ’s (jaw joints). The better and more correct term is TMD which represents temporomandibular disorders. TMD is a series of disorders that can affect the TMJ’s, muscles, nerves. TMD’s have the ability to affect the jaw, teeth, various other intra-oral structures, side of the face, side of the head, back of the head, neck, and upper back. TMD’s can cause headaches, usually tension type but can also be the trigger for migraine headaches. They can cause ear symptoms ranging from pain to ringing to a feeling of fullness in the ears. Often times patients involved in an automobile accident will develop delayed symptoms weeks to months later affecting the ears as well as muscle and joint symptoms. TMD’s can inhibit chewing certain foods due to pain and limited range of motion of the jaw. Another common symptom experienced is a clicking or popping or grating noise when opening and closing the jaw. Actually noises in either joint are common in 40% of the population and need not be addressed unless there is pain associated with the actual noise. Unfortunately, the term TMJ has been used as a catch all term to describe basically anything that can go wrong in the head, neck and face region. What this has led to is misdiagnosis of other possible serious disorders. Some patients have been told they have TMJ when in fact there was something else more seriously occurring. Through his 16 years of treatment Dr. Shannon has diagnosed 3 patients that were told they had TMJ but actually were diagnosed with cancer. These patients had TMJ like symptoms but when examined by Dr. Shannon did not present with symptoms of a typical temporomandibular disorder. When things did not add up as was the case these patients they are referred out to other appropriate specialist for further evaluation. Other disorders diagnosed by Dr. Shannon that were mistaken for TMJ include trigeminal neuralgia which can cause extreme, unbearable pain in the face, giant cell arteritis which is inflammation of arteries usually in the temporal region, and atypical trigeminal neuralgias. Atypical trigeminal neuralgias can cause pain to focus in a tooth or teeth with no apparent cause possibly causing the patient to have the tooth or teeth unnecessarily removed.
When you schedule an appointment for TMD evaluation you will receive a full examination by Dr. Shannon himself along with any imaging (x-rays) that may be necessary. The whole appointment takes approximately 1.5 hours. First Dr. Shannon sits and talks through an extensive history about the present condition. Next, he will perform an actual physical exam in the head, neck, and facial region as well as inside of the mouth. Once a diagnosis is made Dr. Shannon will sit down and explain everything, so the patient fully understands the condition along with going over the treatment options in depth. It is extremely important the patient understand the condition and treatment options, so questions are encouraged to make sure there is a full understanding. Treatment options can include simple education about the disorder, counseling about the disorder, behavior modification techniques, in-house and at home physical therapy, splint therapy, physical self-regulation techniques, prescription of medications, therapeutic injections, trigger point injections, and possible referral to another specialist. Once treatment options are understood Dr. Shannon will formulate a treatment plan that best fits each individual patient’s personality and comfort level.
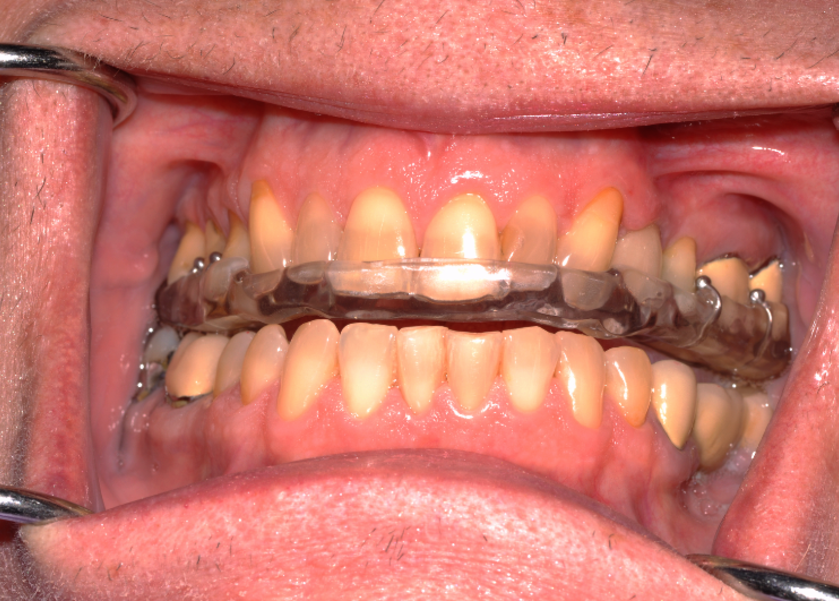


Stretching exercises are taught to increase range of motion of the jaw when jaw muscles limit mouth opening.
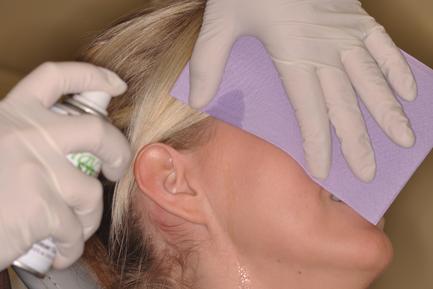
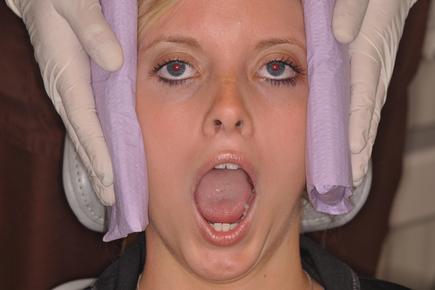
In house physical therapy consists of cold spray followed by heat and gentle stretching. Patients are then taught how to do the therapy at home using frozen gel packs and wet, heated kitchen towel from the microwave oven.